Why and how you can use GalaFLEX™ Scaffold in breast reconstruction?1-5
Examples of how GalaFLEX™ Scaffold (2D or 3D) may be placed
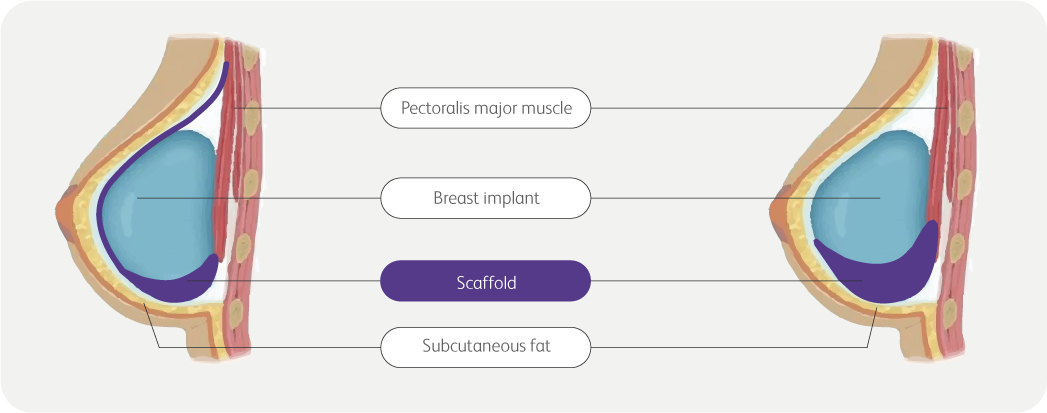
Pre-pectoral*
- Control the breast
pocket and provide
implant support
to reduce implant
malposition.1
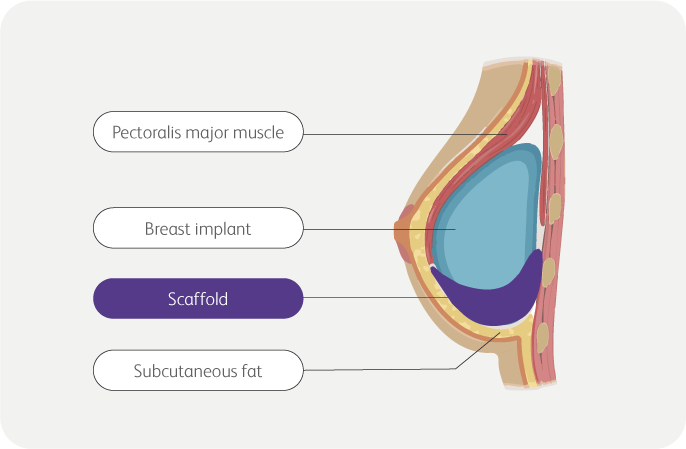
Sub-pectoral*
- Provide extended soft tissue coverage
to the implant or expander.2,6 - Keep the pectoralis muscle in place to
prevent “window-shading”.2,6
*Direct to implant or 2-stage with expander
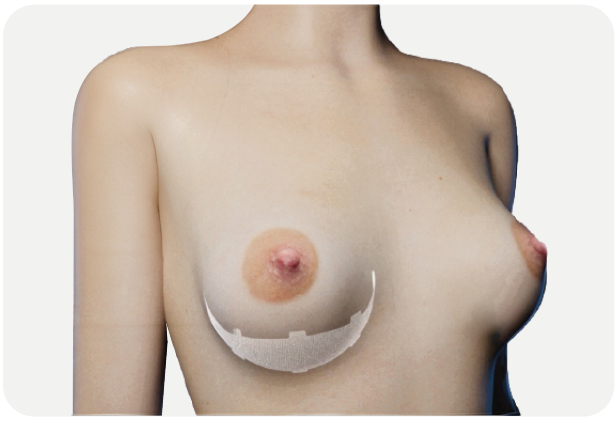
Contralateral breast symmetrization
- Maintain breast shape and position over time by stabilizing the breast internally.7
Clinical studies
in breast cancer reconstruction1,2,3,4,5

- Safe
- Low complication rates
- Used with fat grafting to minimize rippling and scaffold palpability
- Low incidence contracture
- Appears to have equal, if not reduced, capsular contracture rates with when compared with the use od ADM
- Associated with high patient satisfaction
Levy
Poly-4-Hydroxybutyric Acid Mesh Compares Favorably With Acellular Dermal Matrix in Tissue Expander-Based Breast Reconstruction
Levy
Poly-4-Hydroxybutyric Acid Mesh Compares Favorably With Acellular Dermal Matrix in Tissue Expander-Based Breast Reconstruction
Sigalove
Evaluation of the Safety of a GalaFLEX-AlloDerm Construct in Prepectoral Breast Reconstruction
Sigalove
Evaluation of the Safety of a GalaFLEX-AlloDerm Construct in Prepectoral Breast Reconstruction
Movassaghi
Prepectoral Two Stage Implant-Based Breast Reconstruction with Poly-4-Hydroxybutyrate (P4HB) for Pocket Control without the use of Acellular Dermal Matrix (ADM): A 4-Year Review
Movassaghi
Prepectoral Two Stage Implant-Based Breast Reconstruction with Poly-4-Hydroxybutyrate (P4HB) for Pocket Control without the use of Acellular Dermal Matrix (ADM): A 4-Year Review
Bai
Revision Breast Reconstruction With Biologic or Synthetic Mesh: An Analysis of Postoperative Capsular Contracture Rates
Bai
Revision Breast Reconstruction With Biologic or Synthetic Mesh: An Analysis of Postoperative Capsular Contracture Rates
Ruiz Treviño
My experience with direct to implant breast reconstruction using GalaFLEX® An affordable alternative to acellular dermal matrix?
Ruiz Treviño
My experience with direct to implant breast reconstruction using GalaFLEX® An affordable alternative to acellular dermal matrix?References:
1. Movassaghi K, Gilson A, Stewart CN, Cusic J, Movassaghi A. Prepectoral Two-Stage Implant-Based Breast Reconstruction with Poly-4-Hydroxybutyrate for Pocket Control without the Use of Acellular
Dermal Matrix: A 4-Year Review. Plast Reconstr Surg. 2024 Jul 1;154(1):15-24. doi: 10.1097/PRS.0000000000010914. Epub 2023 Jul 6. PMID: 37410610.
2. Levy AS, Bernstein JL, Xia JJ, Otterburn DM. Poly-4-Hydroxybutyric Acid Mesh Compares Favorably With Acellular Dermal Matrix in Tissue Expander-Based Breast Reconstruction. Ann Plast Surg. 2020 Jul;85(S1 Suppl 1):S2-S7. doi: 10.1097/SAP.0000000000002339. PMID: 32243319.
3.Sigalove S, O’Rorke E, Maxwell GP, Gabriel A. Evaluation of the Safety of a GalaFLEX-AlloDerm Construct in Prepectoral Breast Reconstruction. Plast Reconstr Surg. 2022 Oct 1;150:75S-81S. doi: 10.1097/PRS.0000000000009520. Epub 2022 Sep 28. PMID: 35943912.
4. Bai J, Ferenz S, Fracol M, Kim JY. Revision Breast Reconstruction With Biologic or Synthetic Mesh: An Analysis of Postoperative Capsular Contracture Rates. Aesthet Surg J Open Forum. 2024 May 16;6:o-jae035. doi: 10.1093/asjof/ojae035. PMID: 38854738; PMCID: PMC11160324.
5. RUIZ-TREVINO, Juan José. Uso de malla GalaFLEX® en reconstrucción mamaria inmediata con implantes. Experiencia personal. ¿Una alternativa costeable a las matrices dérmicas?. Cir. plást. iberolatinoam. [online]. 2024, vol.50, n.1, pp.19-26. Epub 23-Mayo-2024. ISSN 1989-2055. https://dx.doi.org/10.4321/s0376-78922024000100008.
6. Faulkner, H. R., Shikowitz-Behr, L., McLeod, M., Wright, E., Hulsen, J., & Austen, W. G., Jr (2020). The Use of Absorbable Mesh in Implant-Based Breast Reconstruction: A 7-Year Review. Plastic and reconstructive surgery, 146(6), 731e–736e. https://doi.org/10.1097/PRS.0000000000007384.
7. Wallace L, Wokes JET. Internal Bra: A literature Review and Sub-Classification of Definitions. Aesthetic Plast Surg. 2024 Sep;48(17):3298-3303. doi: 10.1007/s00266-023-03802-4. Epub 2024 Jan 8. PMID: 38189817.